Modern health mapping shows how poverty and ill health persist over 100 years
Researchers from Queen Mary, University of London are aiming to improve the health of Londoners by combining a century-old mapping technique with up-to-the-minute technology.
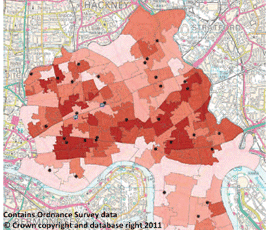
Using type 2 diabetes as their example, the researchers have compiled detailed maps of east London highlighting the geographical ‘hotspots’ of disease risk.
The maps, which are published today in BMJ Open reveal startling similarities to the renowned ‘poverty maps’ created in the late 19th Century by Victorian reformist, Charles Booth.
The researchers chose to study type 2 diabetes risk because it has well-known risk factors and is preventable. It is strongly associated with poverty and South Asian ethnicity, both of which are common in east London today.
The aim of the project is to help local authority and NHS services to tackle poor health by directing efforts where they are most needed. Although the study examined the London boroughs of Tower Hamlets, Hackney and Newham, the researchers say that the same technique could be applied anywhere in the country, and to other diseases.
Unlike the Booth maps which were based on observation, the new study uses an entire set of electronic records from GP surgeries in the area. This very precise information means that the maps are much more accurate and will be useful to individual GP surgeries.
Electronic records from over half a million people were included in the research. Each was assessed for risk of developing diabetes using a well-established prediction tool, the QDScore.
People were categorised as ‘high-risk’ if they were found to have a one in five or greater risk of developing diabetes within ten years.
Overall around ten per cent of the adult population fell into the high-risk category. However the maps showed ‘hotspots’ where up to 17 per cent were at high risk. Further analysis showed that these hotspots were associated with areas of poverty.
These hotspots were surprisingly similar to areas of poverty highlighted in Booth’s maps from over 100 years ago.
The study was led by Douglas Noble, a Public Health Doctor and Lecturer at Barts and The London Medical School, Queen Mary, University of London, and published in BMJ Open with additional material in a full report aimed at the NHS and Public Health specialists.
Dr Noble said: “It was no surprise to see that diabetes risk is high in areas where poverty was high. What was surprising was that some of these pockets of deprivation and ill-health have persisted for over 100 years.
“But unlike in Booth’s time, we now know how diseases like diabetes can be prevented. Using electronic records to create maps like these throughout the country could improve health and save money for the NHS.
“When you think of what life was like in the East End in the late 1800s it’s extraordinary what the NHS and public health professionals have achieved, often with limited resources. But there’s more still to do, and we hope this detailed information will help to reduce risk of diseases like diabetes”
The research also looked at known risk factors and could show where a lack of green space or a proliferation of fast food outlets could be contributing to ill-health.
Trisha Greenhalgh, Professor of Primary Health Care at Queen Mary, University of London, also worked on the report. She said: “Health mapping has enormous potential for the NHS, especially with a disease like type 2 diabetes which we know can be prevented by keeping a healthy weight and staying active.
“This study, which concentrates on three of the ‘Olympic boroughs’, highlights the dire need for a major and lasting Olympic legacy to improve health and longevity in east London.”
Steven Cummins Professor of Urban Health at Queen Mary’s School of Geography commented: "Population health has vastly improved over the last 100 years. However, as these maps starkly illustrate, a century of social, economic and physical change has failed to eliminate underlying geographical inequalities in disease in east London."
This work was funded by Tower Hamlets, Newham, and City and Hackney primary care trusts and by the National Institute for Health Research. The National Information Governance Board advised on data protection issues.
Related items

4 July 2025
For media information, contact:






