Cell ‘battery’ found to play central role in neurodegenerative disease
A devastating neurodegenerative disease that first appears in toddlers just as they are beginning to walk has been traced to defects in mitochondria, the ‘batteries’ or energy-producing power plants of cells.
This finding by researchers at Queen Mary, University of London and Montreal Neurological Institute and Hospital - The Neuro - at McGill University, is published in this week’s issue of the Proceedings of the National Academy of Sciences of the USA.
The disorder, Autosomal Recessive Spastic Ataxia of Charlevoix-Saguenay (ARSACS), primarily affects the cerebellum, a center for movement coordination in the brain. It was first identified in the late 1970s in a large group of patients from Quebec in Canada.
ARSACS strikes at an early age. Symptoms, which worsen over time, include poor motor coordination, spastic stiffness, distal muscle wasting, uncoordinated eye movements and slurred speech. Most patients with the disease are wheelchair-bound by their early 40s and have a reduced life expectancy. ARSACS is not unique to French-Canada as scientists have now found over 100 separate mutations in people worldwide including, including patients in the UK.
The research significantly increases understanding of the disease and reveals an important common link with other neurodegenerative diseases, providing renewed hope and potential new therapeutic strategies for those affected around the world.
“This finding is the most important discovery about ARSACS since the identification of the mutated gene because it gives an indication of the underlying cellular mechanism of the disease,” says Dr Paul Chapple, cell biologist at Barts and The London Medical School, Queen Mary, University of London. He adds: “This work is an essential first step towards developing therapeutic strategies for ARSACS.”
In 2000, scientists identified the gene associated with the disease, which produces a massive 4,579 amino acid protein called sacsin, but until now the role of the sacsin protein has been unknown.
The multi-institutional collaborative research led jointly by Dr Paul Chapple at Queen Mary and Dr Bernard Brais and Dr Peter McPherson in Montreal indicates that that the sacsin protein has a mitochondrial function, and that mutations causing the this ataxia are linked to a dysfunction of mitochondria in neurons.
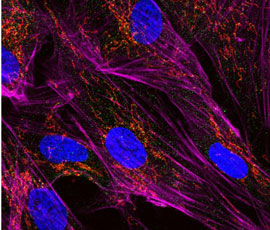
By studying neurons in culture as well as in knockout mice (which do not produce sacsin), the team found that loss of the sacsin protein results in abnormally shaped and poorly functioning mitochondria. In cells mitochondria are constantly fusing together and dividing, with loss of sacsin causing this network to become more interconnected. This disruption led to defective changes in and eventual death of the neurons. In the knockout mice, these disruptions led to neuron death specifically in the cerebellum, suggesting that this is the basis for the neurodegenerative impairments suffered by ARSACS patients.
“Mitochondrial dysfunction has also been identified in major neurodegenerative diseases such as Parkinson, Alzheimer, and Huntington diseases,” says Dr McPherson. “This common link means that research being done on a large-scale on these other diseases may prove critically informative to rarer neurological diseases such as ARSACS, and the inverse may be true, our findings may be fundamental to the study and treatment of other neurodegenerative diseases.”
Dr Chapple adds: “These links between ARSACS and more common neurodegenerations underline the value of studying rare diseases”.
Dr Chapple is funded by the UK Medical Research Council (www.mrc.ac.uk). This research was also supported by the Ataxia Charlevoix-Saguenay Foundation (http://www.arsacs.com/) and the Neuromuscular Research Partnership Program of the Canadian Institutes of Health Research.
Related items

21 August 2025
For media information, contact:

