Tackling the future of Public Health in Pakistan
How can we confront the public health challenges facing Pakistan and the wider region in 2022 and beyond?

A doctor attends to a child in Pakistan
In our latest global seminar, a panel of experts addressed and found solutions for a range of public health challenges. In doing so they spelt out tangible answers for inequality in Pakistan and around Queen Mary's campuses in East London, including the impact of the Covid-19 pandemic and its effect on public health.
The event also discussed:
- Queen Mary's work on mental health in Pakistan.
- How to engage with mental health challenges such as the long-term trauma caused by the coronavirus pandemic.
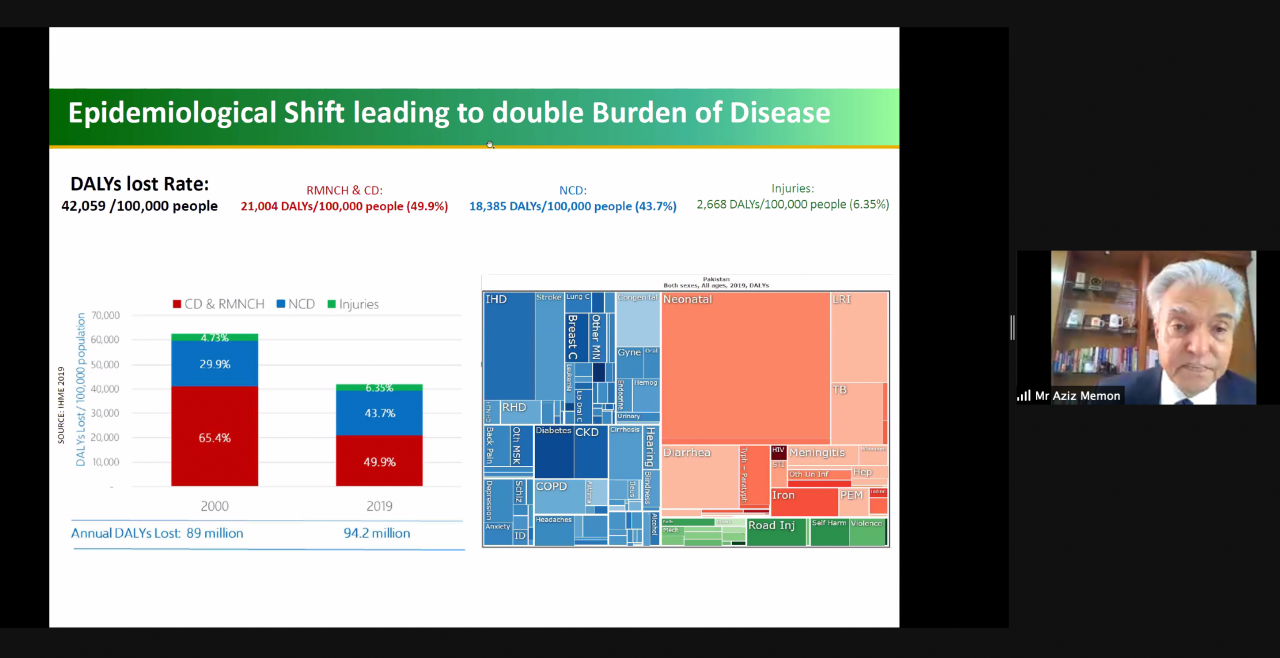
- The impact of non-communicable diseases, nutrition and cardiovascular disease on public health outcomes.
2022 brings cautious optimism as the world continues to adjust and adapt to COVID-19. There are without doubt challenges facing Public Health in Pakistan this year, a scene that is similar across the globe.
The lasting impression this event gave was that there are clear and decisive actors in this area with clear and robust strategies in place to harbour resilience, push through testing encounters and emerge stronger armed with vital lessons for the future.
Facing challenges, ambitions realised
The introduction that welcomed attendees to this pertinent discussion came from Professor Colin Grant Vice Principal (International), Queen Mary University of London.
Professor Irene Leigh, cancer researcher at Queen Mary University of London's Faculty of Medicine and Dentistry, then set out the format of the event with five swift and incisive presentations from our international panel.
In his opening presentation Mr Aziz Memon, Trustee, The Rotary Foundation (2020-24), Pakistan National Polio Plus Committee Chairman and Chairman of the King's Group of Companies clearly set out the challenges Pakistan faces including:
- Weak governance in the financial sector.
- Low financial allocation for health (1% of GDP in the public sector).
- Inadequate access to “universal healthcare/quality of care”.
- A crisis in health workforce.
- Frequent health emergencies.
- Addressing detriments of health.
- Harnessing research and innovation.
These far-reaching and concurrent challenges require an overarching strategy that incorporates a variety of solutions across policy, different sectors and key stakeholders.
The result is an approach that positively disrupts inequality through innovation and behaviour change:
- Enhance Financing for Health.
- Expand Health Services based on Universal Healthcare/ Benefit package.
- Ensure availability of Health Workforce with proper skill mix.
- Tackle Nutrition Crisis.
- Improve Quality of services.
- Strengthen inter-sectoral collaboration.
- Promote culture of evidence-based decision making.
There is a specific target to attain universal healthcare for an additional 46 million people in Pakistan by 2023, an increase of 45% with this figure rising to 55% by 2030.
Tower Hamlets – Tackling Inequality
Next, we were transported to Tower Hamlets where significant health inequalities had resulted due to socioeconomic deprivation.
Three major causes of death in this borough that are linked to health inequalities include:
- Cancer.
- Cardiovascular Disease.
- Chronic Respiratory Disease.
Having set out the challenges faced in the surrounding area of Tower Hamlets, Professor Irene Leigh, cancer researcher at Queen Mary University of London's Faculty of Medicine and Dentistry highlighted a host of initiatives as part of Queen Marys aim to be the most diverse University in the world:
Education
- Enhancing and supporting education engagement from local community.
- Apprenticeship programmes, Initiatives in local area: Institute of Technology.
Research
- Commitment to addressing Health inequalities especially cardiovascular, cancer, population research (public health and primary care).
- New initiatives in “Lifelong health”, “Health Data Science”,” Crisis Prevention” and “Environment and Health”.
Covid-19 Impact and policy challenges
Dr Arjanne Rietsema, Health Specialist at UNICEF Regional Office for South Asia, set out in no uncertain terms the impact of Covid-19, with a 60% reduction of coverage for key maternal and child health interventions as a result of the impact of the Coronavirus.
This disruption in essential health services may result in additional maternal and child deaths. There is also the risk of an increase in early marriages for girls who drop out from school, which could result in additional adolescent pregnancies and low birth weight births.
In order to address these issues, she highlighted some key solutions:
- Sustaining public financing for social services. Protect SDG gains.
- Resilient health systems.
- Equity.
- Building and sustaining social capital (Engagement, Accountability, Ownership, Trust).
- Health in all policies (multi-sectoral).
A multi-disciplinary collaboration to tackle health challenges
The next presentation highlighted the work of the Wolfson Institute of Population Health in relation to non-communicable diseases and came from a trio of speakers.
- Professor Fiona Walter, Professor of Primary Care Cancer Research and Director of Wolfson Institute of Population Health, Faculty of Medicine and Dentistry, Queen Mary University of London.
- Professor Victoria Bird, Professor of Mental Health Care, Acting Head of Unit for Social and Community Psychiatry, Deputy Centre Lead - Centre for Psychiatry and Mental Health, Wolfson Institute for Population Health, Queen Mary University of London.
- Professor Ranjit Manchanda, Professor of Gynaecological Oncology and Consultant Gynaecological Oncologist Wolfson Institute of Population Health, Faculty of Medicine and Dentistry, Queen Mary University of London.
The talk included a recent project with the NIHR Global Research & Group in Collaboration with South Africa and Zimbabwe which posed the question:
‘Can we use innovative approaches with digital technologies in primary care and public health to advance early diagnosis of breast, cervical and colorectal cancer in Southern Africa?’
Ongoing and future projects
The final slides of the talk highlighted community projects which are striving to improve public health in the region for 2022 and the future.
These included:
- PIECEs - Improving outcomes for people with psychosis in Pakistan and India - enhancing the Effectiveness of Community-based care.
Aim: To improve the quality of community-based care for psychosis in India and Pakistan by adapting and testing an evidence-based, low-cost and generic approach, and upscaling using participatory arts methodologies and community engagement.
Watch the event again
